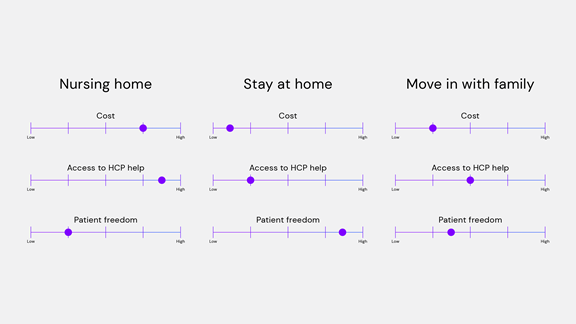
Currently, there is no clear or obvious option for addressing the needs of a person who is aging and has a life-long condition requiring special care.
One option is a nursing home, but this is expensive (avg. £28,000/ yr) and also ‘takes away’ much of the freedom people have enjoyed up to this point. We also have evidence indicating that moving people to a nursing home decreases their life expectancy.
Another common alternative is for the person to continue living at home, which does not constitute an additional cost, but it also does not help with the management of any underlying health conditions.
The other option is for the older person to move in with someone else such as a family member. This option, in theory, addresses both the cost and the health support but is often not practical.
Finally, there is a hybrid between a nursing home and stay-at-home, which involves receiving care at home, either provided by the public system, by social care (reablement), or private care.
There is no obvious good choice. But what if, in the near future, there were other options available to address the needs of the elderly better?
New option 1: Transforming homes into smart care homes
A smart home is an environment with embedded sensors and other devices that seamlessly help the user control elements of their dwelling. These may range from voice-activated lights and thermostats to smart speakers.
The same gadgets could also be used to equip homes with tech that facilitates health monitoring of residents while also promoting independence. The purpose of these devices would be to keep people at home for longer, remain healthier and closely monitor their conditions, effectively reducing the need for out-of-home specialised care.
Current options to add technology to homes focus on increased monitoring (telecare monitoring) or connecting a smart device to a family member or carer. What’s lacking is a ‘prepackaged offer’ suite of options where people can select the level of ‘smartness’ required. This market space would be a fantastic use case for smart tech to bring positive change to people's lives.
New option 2: Fitting nursing and care homes with technology
Another possibility is to fit nursing and care homes with technology and IT systems to help staff provide better care. This may borrow elements of the smart home option, but it expands into the digitisation of records and processes. It incorporates new systems to help staff manage workload whilst freeing time to spend with residents.
These tools have the added benefit of increasing work satisfaction and staff morale. They can save money by automating repetitive tasks and reducing attrition rates. In the private sector, tools such as ERP, CDP and CRM are nothing new, and they work very well. Could we borrow a page from that playbook and use it in this setting?
New option 3: Smart retirement village
The third - and more transformative - option is the concept of a smart retirement village. This borrows elements from the two previous options. Residents live in their own homes without the need to move into a care home, allowing for a greater level of independence and autonomy. They have quick access to health services (GP surgeries and health clinics) as well as other amenities such as recreational facilities, cafes, and other offers to promote active living.
This will not be a budget option, but if structured as a leasehold, it can be seen as an asset, where people buy their home and pay a service charge to the operators of the village. These homes would be fitted with varying levels of tech bespoke to the person's needs or requirements. Built from the ground up with integrated systems working in harmony with one another, rather than bolt-on solutions or through the retrofitting of existing homes. The great side benefit is that it helps to address loneliness.